Research Article - (2025) Volume 9, Issue 1
Received: 24-Sep-2024, Manuscript No. PACN-24-21606 ; Editor assigned: 26-Sep-2024, Pre QC No. PACN-24-21606 (PQ); Reviewed: 10-Oct-2024, QC No. PACN-24-21606; Revised: 13-Feb-2025, Manuscript No. PACN-24-21606 (R); Published: 20-Feb-2025, DOI: 10.35248/ipacn-9.1.32
Objective: To evaluate the efficacy and safety of fluoroscopic-guided repositioning of Peritoneal Dialysis (PD) catheter using guidewire manipulation in our center from Hong Kong.
Methods: All patients underwent fluoroscopic-guided peritoneal dialysis catheter repositioning in our institution between 1st November 2017 to 31st December 2022 were reviewed. Patients fulfilling the selection criteria were identified, with their clinical notes, relevant radiological reports, interventional images and operative records retrospectively reviewed. The success rate was evaluated, with the technical success defined as improved contrast spillage, or return of continuous steady stream after test injection of normal saline immediately after repositioning; clinical success defined as functional peritoneal dialysis catheter after 30 days of repositioning. Logistic regression models were applied to evaluate the variables associated with successful manipulation. Post manipulation complications and the PD time gained after successful manipulation were also reviewed. Results: 46 patients were identified and 54 procedures were performed over the study period. 35 of the interventions (64.8%) resulted in technical success, and 25 cases (46.3%) resulted in clinical success. The median extra PD time gained after successful manipulation was 619 days (IQR, 313.5-1007); (range, 110-1872). The median for number of days of hospital stay after the procedure was 2.5 days (IQR, 2-5), (range, 1-65). 7 cases (13.0%) developed immediate complications, with most cases being peritonitis (n=5), and all were successfully treated with intraperitoneal antibiotics. There was no associated mortality. Objective: To evaluate the efficacy and safety of fluoroscopic-guided repositioning of Peritoneal Dialysis (PD) catheter using guidewire manipulation in our center from Hong Kong.
Methods: All patients underwent fluoroscopic-guided peritoneal dialysis catheter repositioning in our institution between 1st November 2017 to 31st December 2022 were reviewed. Patients fulfilling the selection criteria were identified, with their clinical notes, relevant radiological reports, interventional images and operative records retrospectively reviewed. The success rate was evaluated, with the technical success defined as improved contrast spillage, or return of continuous steady stream after test injection of normal saline immediately after repositioning; clinical success defined as functional peritoneal dialysis catheter after 30 days of repositioning. Logistic regression models were applied to evaluate the variables associated with successful manipulation. Post manipulation complications and the PD time gained after successful manipulation were also reviewed.
Results: 46 patients were identified and 54 procedures were performed over the study period. 35 of the interventions (64.8%) resulted in technical success, and 25 cases (46.3%) resulted in clinical success. The median extra PD time gained after successful manipulation was 619 days (IQR, 313.5-1007); (range, 110-1872). The median for number of days of hospital stay after the procedure was 2.5 days (IQR, 2-5), (range, 1-65). 7 cases (13.0%) developed immediate complications, with most cases being peritonitis (n=5), and all were successfully treated with intraperitoneal antibiotics. There was no associated mortality.
Conclusion: Fluoroscopic-guided repositioning of the peritoneal dialysis catheter was found to be a useful and safe treatment option for malfunctioned peritoneal dialysis catheter and could potentially spare patients from the conventional operative intervention.
Fluoroscopic guided reposition; Peritoneal dialysis catheter; Manipulation; Double-wire technique
Peritoneal Dialysis (PD) is a type of renal replacement therapy for patients with end stage renal disease utilizing the peritoneal cavity to remove waste products from patients. According to renal registry in Hong Kong, more than 86% of new patients requiring dialysis are put on PD. In 2013, there were total of 3817 patients on PD in Hong Kong [1].
However, there are peritoneal dialysis catheter related complications including peritonitis, exit site and tunnel infection, catheter leaks, hernias, outflow obstruction etc. [2]. According to a study in by Mujais S, et al. in 2006, mechanical failure of the PD catheter is the third leading cause of catheter failure among prevalent PD patients [3].
Conservative methods are usually employed first to treat malfunctioning catheters such as postural change, saline infusion and laxatives. If conservative management fails, catheter manipulation including urokinase injection, surgery and wire manipulation would be the management options [6-7]. Among the above treatment options, fluoroscopic guided guidewire manipulation of malpositioned PD catheters has been advocated as a method of catheter salvage in some centers. It is a relatively simple and less invasive procedure compared with traditional laparotomy for management of PD catheter malfunctioning. Patients undergoing fluoroscopic manipulation are likely to have a shorter hospitalization stay and recovery time, and avoiding unnecessary general anesthetic and major operation risks. However, there are limited literatures concerning the efficacy and safety on this technique, especially for patients in our locality [8,9].
Aim
The aim of the study is to review the efficacy and safety of fluoroscopic-guided repositioning of PD catheter using guidewire manipulation in our center.
Procedure
For fluoroscopic guided catheter repositioning in our centre, the PD catheters and exit sites are prepared in meticulous sterile fashion. It is usually done under minimal or conscious sedation, with administration of intravenous sedatives or analgesics, commonly midazolam or fentanyl in our unit, depending on patient’s tolerance and duration of the procedure.
At the start of the procedure, a small amount of diluted contrast is gently injected into the PD catheter under fluoroscopic screening to look for: 1) Catheter patency, and 2) The spillage pattern of the contrast in the peritoneal cavity, to determine whether there is contained or free spillage. A guidewire is then passed through the catheter into the peritoneal cavity, and is advanced until encountering initial resistance, usually from contact between the guidewire and the bowel, mesentery, or diaphragm. Usually the catheter will begin to buckle and back-out of its original position. With continuous advancement of the guidewire, the catheter will start to shift position. If necessary, “double-wire technique” with an additional guidewire insertion into the same PD catheter could be performed, providing extra support to reposition the catheter tip. The above steps are repeated until successful repositioning, or until it is apparent that repositioning cannot be achieved after multiple attempts (Figures 1-3).
Figure 1: (A) Showed initial PD catheter tip position at lower abdomen/pelvis (arrow). There was contained contrast spillage shown in Figure (B) at the start of procedure (circle).
Figure 2: (A) and (B) Showed advancement of a guidewire until resistance encountered, with the PD catheter began to buckle and back-out of its original position.
Figure 3: Showed successful repositioning of the catheter tip to an upper position (arrowhead).
The procedure would be considered as technical success if either, 1) There is improved contrast spillage on fluoroscopic screening, or 2) Return of continuous steady stream after test injection of normal saline immediately after repositioning (Figure 4).
Figure 4: The performing radiologist was injecting small amount of normal saline into the catheter immediately after repositioning for test injection in Figure 4(A). Figure 4(B) showed return of a continuous and steady stream (arrow), suggesting technical success.
This retrospective study in a single institution was approved by the Research Ethics Committee (Kowloon Central/Kowloon East). Patients underwent fluoroscopic-guided peritoneal dialysis catheter repositioning in Department of Diagnostic and Interventional Radiology in Kwong Wah Hospital from 1st November 2017 to 31st December 2022 were identified via Radiology Information System (RIS) and included in this study. Patients with no definite evidence of mechanical PD catheter failure upon arrival in intervention radiology suite, no clinical follow up 30 days after catheter repositioning or no available image of catheter repositioning procedure in Picture Archiving and Communication System (PACS) were excluded.
After reviewing the patient clinical notes, radiological reports and operative records from Electronic Patient Record (EPR) and relevant interventional images from PACS, the following data was collected:
Patients’ Demographics
Age, gender, number of previous intra-peritoneal surgeries before PD catheter manipulation and duration of the latest PD catheter inserted before manipulation.
Procedure Details
Indication for revision, i.e., being primary catheter failure, which was defined as immediate PD catheter failure after insertion, or secondary catheter failure, which was defined as catheter failure after previous successful PD, the date of catheter manipulation, number and type of guidewire(s) used, pre and post-procedural PD catheter tip positions, and any change in quadrant of the catheter tip position in post procedural fluoroscopic images.
The PD catheter tip position was divided in four abdominal quadrants by an imaginary horizontal line between the iliac crests and a vertical line at midline of abdomen along the spinous processes in fluoroscopic images (Figure 5). The relevant fluoroscopic images were reviewed by a senior radiologist with dedicated training in interventional radiology (with 6 years of post-fellowship experience to interventional radiology) who was blinded to patients’ demographics and procedure outcome. The pre and post-procedural PD catheter tip positions, and any change in quadrant of the catheter tip position in post-procedural fluoroscopic image were determined.
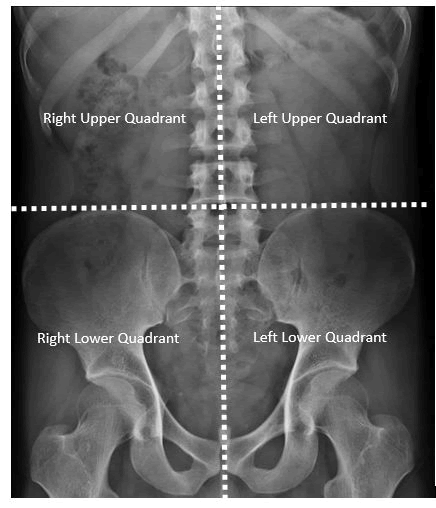
Figure 5: Defined the PD catheter tip position into four abdominal quadrants, by an imaginary horizontal line between the iliac crests and a vertical line at midline of abdomen along the spinous processes in fluoroscopic images (as dotted lines).
Outcome
Technical success, which was defined as: 1) Improved contrast spillage, or 2) Return of continuous steady stream after test injection of normal saline immediately after repositioning. Technical failure was defined as failure to demonstrate both improved contrast spillage on fluoroscopic screening and return of continuous steady stream after test injection of normal saline immediately after repositioning. If there was no clear documentation of contrast spillage or free stream flow upon saline injection in the radiology report, it would be categorized as technical indeterminate. Clinical success was defined as functional peritoneal dialysis catheter after 30 days of repositioning. Immediate post manipulation complications, subsequent management for non-success cases, including intra-operative findings for patients underwent laparoscopic manipulations were also included. For clinically successful cases, post manipulation successful extra PD time gained and days of hospital stay after the procedure were also included. The extra PD time gained was defined as the additional time PD remained functioning after clinically successful fluoroscopic repositioning, with endpoint being PD catheter failure, patient’s death or the date of data collection.
Statistical Analysis
Logistic regressions were applied for the analysis of factors associated with clinical success using IBM SPSS Statistics, including gender, age, the pre and post-procedural catheter tip positions, change in quadrant of catheter tip position in post procedural fluoroscopic images, indication for manipulation (primary vs. secondary catheter failure), duration of PD catheter inserted before manipulation, and number of intra-peritoneal surgeries before manipulation. A P-value of ≤ 0.05 was considered as statistically significant. A Kaplan-Meier survival curve of functioning PD catheter after clinically successful fluoroscopic manipulation was plotted to determine the extra PD time gained after the procedure.
Patient Demographics
56 cases fulfilling the inclusion criteria were initially identified via RIS. 2 cases were excluded as they showed satisfactory contrast spillage and steady stream return upon saline injection in interventional radiology suite before the start of manipulation, suggesting a patent and functional PD catheter. A final 54 procedures from 46 patients performed during the period from 1st November 2017 to 31st December 2022 were included. 33 cases (61.1%) were male patients. The mean age at the time of procedure was 63.6 ± 13.8 years old (± Standard Deviation/SD). All the PD catheters involved were Covidien straight tip Tenckhoff catheters (42 cm). 21 procedures (38.9%) were arranged due to primary failure of the catheter, while 33 cases (61.1%) were due to secondary failure. 43 cases (79.6%) had not undergone any intra-peritoneal surgery before PD catheter manipulation. 11 cases (20.4%) had at least one intra-peritoneal surgery before catheter manipulation, maximum up to 3 times. The median duration of the latest PD catheter inserted before manipulation was 76 days (interquartile range/IQR, 37-545), (range, 6-3065). Patient demographics were summarized in Tables 1 and 2.
Procedure
The type of guidewires used included Terumo, Stiff Terumo, Amplatz, Cordis Emerald and Roadrunner. In 35 cases (64.8%), a combination of two or more types of guidewires were used for manipulation, with the commonest combination being Terumo plus Terumo Stiff guidewires, accounting for 18 cases (33.3%). Maximum number of guidewires used was up to 3 in each procedure (Figure 6). All procedures were performed by at least one radiologist with dedicated training in interventional radiology (ranging from 1 year to 14 years of post-fellowship experience to interventional radiology at the time of performing procedure).
Figure 6: Types and combinations of guidewires used.
The pre and post-manipulation PD catheter tip positions were also documented and summarized in Tables 1 and 2. In 34 cases (63.0%), there was a shift in quadrant of the final catheter tip position compared to pre-procedural position.
| Value | |
| Gender | |
| Male | N=33 (61.1%) |
| Female | N=21 (38.9%) |
| Mean age (year ± SD) | 63.6 ± 13.8 |
| Number of intra-peritoneal surgery before catheter reposition | |
| 0 time | N=43 (79.6%) |
| 1 time | N=8 (14.8%) |
| ≥ 2 times | N=3 (5.6%) |
| Median duration of the latest PD catheter Inserted before reposition (day) | 76 (IQR, 37-545); (range, 6-3065) |
| Indication for reposition | |
| Primary catheter failure | N=21 (38.9%) |
| Secondary catheter failure | N=33 (61.1%) |
| Pre-manipulation catheter tip position | |
| Right upper quadrant | N=8 (14.8%) |
| Left upper quadrant | N=9 (16.7%) |
| Right lower quadrant | N=17 (31.5%) |
| Left lower quadrant | N=20 (37.0%) |
| Post-manipulation catheter tip position | |
| Right upper quadrant | N=4 (7.4%) |
| Left upper quadrant | N=6 (11.1%) |
| Right lower quadrant | N=17 (31.5%) |
| Left lower quadrant | N=27 (50.0%) |
Table 1: Patient demographics (Combined).
|
|
Primary failure (n=21) |
Secondary failure (n=33) |
|
Gender |
||
|
Male |
N=12 (57.1%) |
N=21 (63.6%) |
|
Female |
N=9 (42.9%) |
N=12 (36.4%) |
|
Mean Age (year ± SD) |
65.1 ± 13.9 |
62.6 ± 13.7 |
|
Number of intra-peritoneal surgery before catheter reposition |
||
|
0 time |
N=18 (85.7%) |
N=25 (75.8%) |
|
1 time |
N=2 (9.5%) |
N=6 (18.2%) |
|
≥ 2 times |
N=1 (4.8%) |
N=2 (6.0%) |
|
Median duration of the latest PD catheter inserted before reposition (day) |
32 (IQR, 7-34); (range, 6-76) |
674 (IQR, 79-1372); (range, 34-3065) |
|
Pre-manipulation catheter tip position |
||
|
Right upper quadrant |
N=3 (14.3%) |
N=5 (15.2%) |
|
Left upper quadrant |
N=1 (4.8%) |
N=8 (24.2%) |
|
Right lower quadrant |
N=10 (47.6%) |
N=7 (21.2%) |
|
Left lower quadrant |
N=7 (33.3%) |
N=13 (39.4%) |
|
Post-manipulation catheter tip position |
|
|
|
Right upper quadrant |
N=2 (9.5%) |
N=2 (6.0%) |
|
Left upper quadrant |
N=0 (0%) |
N=6 (18.2%) |
|
Right lower quadrant |
N=8 (38.1%) |
N=9 (27.3%) |
|
Left lower quadrant |
N=11 (52.4%) |
N=16 (48.5%) |
Table 2: Patient demographics subcategorized into primary and secondary catheter failure groups.
Outcomes
35 cases (64.8%) resulted in technical success. For 4 cases (7.4%), there was only a change in PD catheter tip position demonstrated in the fluoroscopic images, without clear documentation of contrast spillage or free stream flow upon saline injection so they were categorized as indeterminate for technical success. All these 4 technically indeterminate cases resulted in clinical success. 15 cases (27.8%) were categorized as technical failure cases (Figure 7).
Figure 7: Technical outcomes.
25 cases (46.3%) resulted in clinical success, with 13 cases in primary catheter failure group and 12 cases in secondary catheter failure group. Of the failed 29 cases, 12 were scheduled for subsequent laparoscopic manipulation, 6 were rebooked for another trial of fluoroscopic guided intervention at one to two months’ interval, in which 4 of them achieved a clinical success in the second time of fluoroscopic guided repositioning. 9 were switched to long term hemodialysis and 2 were continued with conservative management due to underlying co-morbidities (Figure 8).
Figure 8: Clinical outcomes.
Among the 12 cases undergone laparoscopic repositioning of the catheter, with most of the cases found to have omental wrapping the catheter (n=6) (Figure 9).
Figure 9: Intra-operative findings of clinical failure cases underwent surgical repositioning.
Among the 25 clinically successful cases, the median of “extra PD lifespan” gained after successful manipulation was 619 days, with maximal extra lifespan up to 1872 days (IQR, 313.5-1007); (range, 110-1872). For 7 cases of the clinically successful group, their PD catheters still remained functional on day of data collection on 1st April 2023, with a median PD time of 858 days (IQR, 619-1115); (range, 311-1872) (Figure 10).
Figure 10: Kaplan-Meier survival curve of functioning PD catheter after clinically successful fluoroscopic manipulation.
The median for number of days of hospital stay after the procedure was 2.5 days, (IQR, 2-5); (range, 1-65). 13 cases (24.1%) were immediately discharged on the next day after procedure (Table 3).
| Result | Ratio (Percentage) |
| Technical success | 35/54 (64.8%) |
| Clinical success | 25/54 (46.3%) |
| Clinical success in primary failure group | 13/21 (61.9%) |
| Clinical success in secondary failure group | 12/33 (36.4%) |
| Median of extra PD catheter lifespan gained after successful manipulation | 619 days (IQR, 313.5-1007 days); (range, 110-1872 days) |
| Median of hospital stay after procedure | 2.5 days (IQR, 2-5 days); (range, 1-65 days) |
Table 3: PD catheter fluoroscopic manipulation outcomes.
Complications
7 cases (13.0%) developed immediate complications, with most cases being peritonitis (n=5). All the 5 peritonitis cases were successfully treated with intraperitoneal antibiotics without other major complications. 1 case developed a small intraabdominal abscess at the tip of PD catheter three days after the procedure, in which concealed bowel perforation was suspected (Figure 11). The patient subsequently underwent ultrasound guided drainage of the abscess, without need of laparotomy. 1 case developed a pseudoaneurysm at a small branch of right inferior epigastric artery, which was managed conservatively with blood transfusion and patient’s vitals and hemoglobin level remained stable (Figure 12). No associated mortality case was identified.
Figures 11: (A) and (B) Showed intra-abdominal abscess formation around the PD catheter tip, with internal gas locules and adjacent inflammatory changes. (circles) Patient underwent ultrasound guided drainage of the abscess and was later discharged.
Figure 12: (A) and (B) Showed a tiny pseudoaneurysm at a small branch of right inferior epigastric artery (circles), with adjacent hematoma at right anterior abdominal wall. Patient was treated conservatively with blood transfusion.
Predictors of Success
Factors associated with final clinical success were analyzed by binary logistic regression using IBM SPSS, including patient’s gender, age at manipulation, indication of catheter revision (primary vs. secondary catheter failure), initial catheter tip position before manipulation, immediate post manipulation catheter tip position, change in quadrant of final catheter tip position compared to pre-procedural tip position, any intraperitoneal surgeries before manipulation and duration of PD catheter inserted before manipulation. None of the abovementioned factors were able to demonstrate a statistically significant correlation with likelihood of clinically successful outcome, using P value<0.05 as statistically significant result (Table 4).
| Odds ratio (95% CI) | P Value | |
| Univariate analysis | ||
| Age | 1.02 (0.97-1.07) | 0.39 |
| Gender (M vs. F) | 0.34 (0.07-1.61) | 0.17 |
| Indication for PD Catheter Revision (Primary vs. Secondary failure) | 0.62 (0.13-2.86) | 0.54 |
| Pre-procedural catheter tip position | ||
| Right upper quadrant | Reference | |
| Left upper quadrant | 2.44(0.15-39.34) | 0.53 |
| Right lower quadrant | 2.13 (0.22-20.56) | 0.52 |
| Left lower quadrant | 3.74 (0.41-34.04) | 0.24 |
| Post-procedural catheter tip position | ||
| Right upper quadrant | Reference | |
| Left upper quadrant | 0.05 (0.10-1.86) | 0.1 |
| Right lower quadrant | 0.06 (0.11-2.86) | 0.16 |
| Left lower quadrant | 0.19 (0.14-6.10) | 0.35 |
| Change in quadrant of catheter tip position (Yes vs. No) | 0.49 (0.11-2.10) | 0.34 |
| Any intra-peritoneal surgery before manipulation (No vs. Yes) | 0.58 (0.12-2.83) | 0.5 |
| Duration of PD catheter inserted before manipulation (per 10 days) | 0.99 (0.99-1.00) | 0.06 |
Table 4: Logistic regression model of factors associated with clinical success.
In this study of 54 cases with non-functioning PD catheters, fluoroscopic guided repositioning resulted in a technical success in 35 cases (64.8%) and clinical success in 25 cases (46.3%). The previously reported clinical success rates for fluoroscopic manipulation ranged from around 25% to 67%. The clinical success rate in our study was around the midrange, and was comparable to a Korean study by Kwon YH et al. in 2014 with a clinical successful rate of 47% after fluoroscopic catheter manipulation.
The median of extra PD catheter lifespan gained after successful manipulation was 619 days (around 20 months), which was longer than prior studies of fluoroscopic guided repositioning (mean of 278 days), and longer than studies of surgical repositioning (9-16 months). There were 7 cases with their PD catheters still remaining functional on day of data collection in our study, with the longest duration up to 1872 days. In 12 clinically successful cases, the peritoneal dialysis was discontinued as the patient was deceased due to other reasons, with their PD catheter still remaining functional before the time of death. Therefore, the extra PD catheter lifespan gained after fluoroscopic guided catheter manipulation in our study was presumably underestimated.
In our study, there were 7 cases (13.0%) with immediate complications, which was significantly lower than the complication rate in conventional surgical repositioning (up to 39%). The most frequent complication was peritonitis (n=5), with all cases being successfully managed with intraperitoneal antibiotics. No associated mortality case was identified.
With the minimally invasive nature of the procedure and avoidance of general anesthesia compared to conventional surgical repositioning, most of the patients received fluoroscopic guided PD catheter positioning were discharged soon after the procedure, with median for number of days of hospital stay after the procedure being 2.5 days (IQR, 2-5); (range, 1-65). 13 cases (24.1%) were even discharged on the next day after procedure. PD was resumed immediately after procedure for all the technically successful cases.
4 out of the 6 cases who underwent a second trial of fluoroscopic guided intervention finally achieved clinical success. This success rate might indicate that retrying fluoroscopic guided repositioning after an initial failure could be a worthwhile consideration. It might suggest that the procedure has the potential to be successful with further attempts, and that the initial failure might not necessarily be indicative of future outcomes. Nonetheless, more data analysis would be required to verify this hypothesis due to the limited number of cases.
There were a few limitations in our study. The first one would be the small sample size from a single institution. There was a limited patient load as it is not a common practice or routine in our locality, with many of the cases in Hong Kong would directly go to surgical repositioning after failing conservative measures. This might give rise to a possible low statistical power for this study. Another limitation was case selection bias and its retrospective study nature. Not all the cases failing conservative management would be referred to our unit for fluoroscopic guided manipulation, with some cases being referred to surgical laparotomy directly due to various reasons. The cases referred to our unit might be technically less complicated, and contributing to case selection bias and possibility of overestimating the success rate, particularly for the more complex cases.
There is a lack of literatures reviewing the efficacy and safety on this technique in our locality and the result of this local study could support the use of fluoroscopically guided manipulation of malfunctioning PD catheter for our populations. Larger scale studies could be performed for further evaluation, such as the radiation dose for each procedure, procedure techniques, procedural time, patients’ experience in terms of discomfort and pain etc.
Given the satisfactory clinical success rate, lower complication and shorter recovery time compared to conventional surgical approach, fluoroscopically guided manipulation could be considered as a less invasive alternative to surgical laparotomy for cases failing conservative treatment.
Fluoroscopic-guided repositioning of the peritoneal dialysis catheter was found to be a useful and safe treatment option for malfunctioned peritoneal dialysis catheter and could potentially spare patients from the conventional operative intervention.
[Crossref] [Google Scholar] [PubMed]
[Crossref ] [Google Scholar]
[Crossref ] [Google Scholar]
[Crossref ] [Google Scholar]
Citation: Lau RWC, Pan ECW, Wong A, Ho BLK, King CK, et al. (2025) Efficacy and Safety of Fluoroscopic-guided Repositioning for Malfunctioning Peritoneal Dialysis Catheter by Guidewire Manipulation. Ann Clin Nephrol. 09:32.
Copyright: © 2025 Lau RWC, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.