Keywords
Cardiovascular health; Lifestyle; Public health; Mobile health
technology
Introduction
More than 25% of American adolescents and young adults
currently have high cholesterol, high blood glucose, and
hypertension; yet over 75% are unaware of their cardiovascular
risk factors [1]. According to the National Health and Nutrition
Examination Survey, individuals between 18-39 years old have
the lowest hypertension control rates [2]. Late adolescence to
early adulthood is a critical developmental period in establishing
health-related attitudes and behaviours [3]. Lifestyle choices become increasingly consolidated during these years and these
long-term patterns are associated with health outcomes later in
life [3-6]. Thus, research into preventing heart disease beginning
early in life is a major priority in the field.
Lifestyle behaviours including, healthy eating, maintaining a
healthy weight, regular physical activity, and smoking avoidance
are so powerful, that people who do all four can reduce their
risk for all chronic diseases by roughly 80% [7]. In addition to
these more commonly known factors, there are other ways to prevent cardiovascular disease. Spending time with loved ones,
hugging, laughing, and having a pet: all reduce stress, ease
anxiety, and lower blood pressure [8-12]. The benefit of these
simple behaviours has been found to produce a benefit similar to
that seen with statins or aerobic exercise [8]. In particular, sleep
is emerging as a significant target for improving cardiovascular
risk profiles. The American Academy of Paediatrics has deemed
this a “public health epidemic” with immense implications given
the widespread prevalence of chronic sleep deprivation in young
people [13,14]. Studies show that students who obtain less sleep
have lower self-esteem and do not perform as well in school
[14,15]. Further, only 2%-25% of high schoolers get a minimum of 8 hours each night as recommended by the National Sleep
Foundation [16,17].
Providing heart-healthy information and encouraging positive
lifestyle changes in adolescents and young adults are especially
challenging [4]. One study showed that fewer than half of
adolescents received hypertension education from physicians
and of those that did more than half discarded educational hand-
outs as soon as they left the clinic [18]. Limited knowledge and
awareness of cardiovascular risk factors lead to low motivation to
adopt these preventive behaviours, especially when most young
people are generally healthy and do not think about how their
current decisions influence their chances of living with chronic
disease later in life [9].
Mobile health technology, including the use of SMS or text
messaging to facilitate disease prevention, is of growing interest
[19,20]. Text 4 Heart II, was a program that studied how text-
messaging could improve medication adherence among adult
patients with cardiovascular disease [21]. A systematic review of
45 electronic health interventions showed positive effects such
as reducing smoking rates and alcohol intake while improving
nutrition and physical activity in young adults, however, 80% of these were delivered via websites [22]. Text messaging is
widely used among adolescents and young adults in the U.S with
estimates of 86% using a smartphone [22]. According to the Pew
Research Centre young adults (18-24) send or receive an average
of 50 text messages per day [23].
Our study, Early Cardiovascular Health Outreach SMS (ECHOS),
evaluated the effectiveness and feasibility of providing text
messaging as a tool for delivering evidence-based heart-healthy
information to adolescents and young adults. We also aimed to
encourage the practice of simple, yet effective behaviours known
to reduce cardiovascular risk profiles with early adoption in life.
“Nudge theory” is a behavioural science concept, which proposes
that positive reinforcement and indirect suggestions (without
restricting choice) can predictably influence behaviour [24].
Nudge interventions have been applied in British and American
public health policy to change behaviour and are highly appealing
as they are low cost and typically do not require on-going
resources to sustain. [25] We hypothesized that text-messages
would be an effective means of “nudging” participants to reflect
briefly on how well their current behaviour aligns with a heart-
healthy lifestyle and to consider taking action now to improve
their current and future cardiovascular health.
Methods and Design
We performed a multi-phase, prospective, cohort study of
adolescents and young adults between 13 and 25 years of
age. Eligible participants were smartphone owners with a text
messaging plan. Participants received texts on evidence-based
preventive cardiovascular strategies and habits for 30-90 days.
Text messages were crafted by young adults (a medical student
and undergraduate student) with active feedback from faculty
cardiologists (Figure 1). Feedback from a high school student
helped to make the texts as relevant and engaging as possible for
the teen targeted age group. Participants were recruited from U.S.
middle schools, high schools, and colleges via email dissemination
of recruitment materials, as well as in-person recruitment on
the campus of the University of California Los Angeles (UCLA).
Text messages were delivered through a web-based application
called Chorus created at UCLA. All participants were emailed a
survey created with Survey Monkey before and after receiving
ECHOS text messages. The surveys collected demographic data,
used open-ended questions (e.g., hours slept), and 5-point-
rating scales to assess health knowledge. Participation under
the age of 18 required parental consent in addition to standard
personal consent. Each phase was approved by the UCLA Medical
Institutional Review Board (#16-001393) (Figure 1).
Figure 1: A Sample text messages from 3 phases of early cardiovascular
health outreach SMS pilot trials. Each text message was limited to
160 characters. The Chorus app did not support images or emojis.
Data analysis
Quantitative data were analysed using two-tailed t-tests, linear
regression models, and significance levels of p<0.05. At the end
of each phase, the survey also asked participants for feedback
about the ECHOS program. These free-text responses were
qualitatively coded and analysed for themes.
Phase 1
Phase 1 (spring 2018) served as a pilot study to test the platform.
We aimed to enrol at least 20-25 participants after using
Whitehead’s stepped rules of thumb for determining optimal
sample size for a pilot study [26]. This method took into account
the likely size of a future trial designed around a small effect
size (such as 0.2) and desired 80-90% power. Phase 1 consisted
of sending weekly texts (over 90 days) about broad topics
such as smoking cessation, nutrition, physical activity, stress
management, sleep, and heart-healthy habits. Sleep deficiency
was identified as a significant health threat to participants from
Phase 1 of the ECHOS project, supporting the literature that
this is a major targetable approach for improving cardiovascular
health in adolescents and young adults [14-17]. Thus, we focused
on sleep for Phase 2 of ECHOS (summer 2018).
Phase 2
In Phase 2 we sought to hone-in on one topic rather than many
and explore the response to a program with more frequent text-
messages over a shorter total length of time. 14 sleep-specific text
messages were sent to enrolled participants over a period of 30
days. Pre and post-survey responses were analysed for changes
in sleep hygiene knowledge, quantity, and quality of sleep. To
measure the quality of sleep and the extent of sleep disturbances
in this population, we applied the Medical Outcomes Study
(MOS) Sleep Scale-Revised (MOS Sleep–R), which is a previously
validated and reliable tool for assessing psychometric properties
contributing to overall sleep quality [27,28]. Briefly, this includes
questions about the participant’s sleep in the past 3 months
across 3 domains: disturbance, somnolence, and adequacy.
Summing the scores across these domains generates the Sleep
Problems Index (SPI) with higher scores indicating more sleep
problems overall. Using the mean SPI and standard deviation for
a representative sample of the US adult population, an effect size
of at 0.1-0.2 (given that a meaningful change of SPI would be at
least 1.5 points) we estimated needing a sample size of at least
150 participants per arm for a full-scale study [27]. A controlled
trial of this scale did not align with our research team’s goals
at the time and was infeasible (due to lack of funding), so we
decided to proceed with phase 2 and 3 of ECHOS with revised
pilot protocols.
Phase 3
Phase 3 of this project (winter 2019) was the final iteration of
ECHOS pilot testing. Previous research supports the use of the
Lifestyle and Habits Questionnaire-Brief (LHQ-B) [6] to assess
lifestyle behaviours and attitudes in young adults 18-25 [6]. Each
item contained a statement about different lifestyle behaviours
and attitudes. For each item, participants were asked to broadly
examine their own lifestyle behaviours and attitudes, then rate
their level agreement with the given statement (e.g., “I avoid
smoking cigarettes”). The scale ranged from 1 “strongly disagree”
to 5 “strongly agree” with higher scores indicating healthier habits
and attitudes. A modified LHQ-B with six of eight original domains
was adapted for pre and post-surveys, including physical activity,
psychological health, substance use, nutrition, social concern,
and sense of purpose. According to the authors, the LHQ-B
domains of psychological health and social concern were the top
two domains that predicted stress levels [6]. Twenty-four text
messages were sent over a month-long period, and participants
received texts three times a week. $10 Amazon gift cards were
provided to help increase cohort size during this phase.
Results
Recruitment and demographics
ECHOS enrolled a total of 260 participants between 13 and
25 years of age in 3 separate cohorts. The average age was 19
years. There were 195 females, 63 males, and 2 transgender
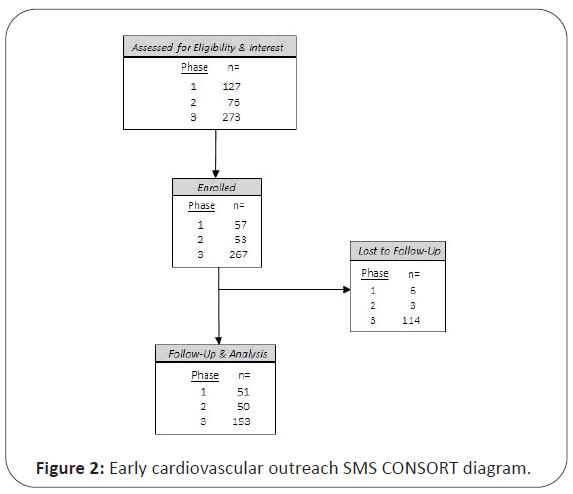
participants. The demographics of participants are shown in Figure 2 and Table 1.
| Characteristics |
| Phase 1 |
Phase 2 |
Phase 3 |
| n=51 |
n=50 |
n=153 |
| Mean age (years) ± SD |
19.6 ± 1.9 |
Mean age (years) ± SD |
19.3 ± 2.94 |
Mean age (years) ± SD |
19.7 ± 1.6 |
| Sex (% Female) |
67% |
Sex (%Female) |
64% |
Sex (%Female) |
82% |
| Race and ethnicity |
Race and ethnicity |
Race and ethnicity |
| Asian or Pacific Islander |
71% |
White, not Hispanic |
46% |
Asian or Pacific Islander |
56% |
| Caucasian |
20% |
Asian or Pacific Islander |
22% |
Caucasian |
23% |
| Hispanic/Latino |
3.50% |
Latino/Hispanic |
14% |
Hispanic/Latino |
11% |
| American Indian/Alaskan |
3.50% |
Black/African American |
6% |
Other multiracial |
10% |
| African American |
2% |
Middle Eastern |
4% |
|
|
| |
|
Other multiracial |
8% |
|
|
| School grade |
School grade |
Year in college |
| Middle school |
1.80% |
Middle school |
2% |
First |
37% |
| High school |
8.80% |
High school |
9% |
Second |
22% |
| College |
75.40% |
College |
75% |
Third |
12% |
| Other |
14% |
Other (graduate school) |
14% |
Fourth |
22% |
| |
|
|
|
Graduate |
13% |
Table 1: Recruitment results for each of the 3 Phases of ECHOS.
Figure 2: Early cardiovascular outreach SMS CONSORT diagram.
Individuals completed interest forms which prompted them
to verify their eligibility and provide their contact information.
They (or their parents for participants under 18 years old) were
then emailed the consent form. Enrolled participants were
those that consented to begin receiving ECHOS text messages
and completed the pre-intervention survey. Follow-up included
completion of the post-intervention survey, which contained the
same questions but also asked for feedback about the ECHOS
program. In the third phase, there were a disproportionate
number of participants that did not complete the post-survey.
This may have been due to the survey being sent during final
examination of the academic quarter at the university. Only
participants that responded to both pre- and post-intervention
surveys were included in analyses.
Phase 1
Pre-intervention results: Pre-intervention surveys established
a baseline by asking participants about their behaviours, on
average, over the past 3 months. At baseline participants “felt
stressed” or “had trouble relaxing” about 50% of the time. The
reported average nightly hours of sleep were 6.5 ± 1.7 hours and
participants felt they received enough sleep only 50% of the time.
Pre-intervention surveys demonstrated that few participants
(12.2%) smoked cigarettes or e-cigarettes. Participants reported a
high level of attention to portion size during meals and reported
consuming a low-fat diet “some of the time,” on average.
Participants reported an average of 6-10 days of exercise over
the past 3 months. On average, adolescents and young adults
felt somewhat knowledgeable about heart disease, cancer,
and nutrition. The internet was the most cited source of health
information (73%), followed by family and physicians (22%), and
finally schools (5%).
Post-intervention results: Thirteen text-messages were sent
over 90 days. Overall, participants reported that they read the
text messages “most of the time.” The ECHOS program resulted
in an increase in heart knowledge by 16% [p=0.004]. There was a
21% [p=0.007] increase in perception of heart disease prevention knowledge by the end of the intervention, corresponding to
“somewhat knowledgeable” on the Likert scale. There was also
a 19% [p=0.02] increase in how often participants thought about
portion sizes and a 21% [p=0.03] increase in how often they ate
a low cholesterol diet. There was no significant difference in
nutrition knowledge, sense of happiness, stress, sleep quality,
and exercise. Interestingly, our early results showed that tobacco
smoking and vaping interventions were less relevant in this
sample; but rather there was a need to address sleep and stress
management.
For heart disease and nutrition, surveys used the following scale
of 1 is not knowledgeable, 2 is somewhat knowledgeable, and 3 is
very knowledgeable. Participants answered the question “do you
know how to prevent heart disease?” with a scale of 1 being no,
2 being some of the time, 3 being half of the time, 4 being most
of the time, and 5 being yes. There was a statistically important
increase in heart disease knowledge from not knowledgeable to
somewhat knowledgeable and heart disease prevention from
knowing how to prevent heart disease some of the time to half
of the time (Table 2).
| |
Pre-intervention |
Post-intervention |
p-value |
| Where do you rank yourself about your knowledge on heart disease? |
1.8 ± 0.3 |
2.1 ± 0.3 |
0.004 |
| Where do you rank yourself about your knowledge on nutrition? |
2.2 ± 0.4 |
2.17 ± 0.3 |
0.6 |
| Do you know how to prevent heart disease? |
2.9 ± 1.5 |
3.5 ± 0.7 |
0.007 |
Table 2: ECHOS Phase 1: Health knowledge.
Adolescents and young adults were asked how often questions
using the following scale of 1 is never, 2 is some of the time, 3 is
half of the time, 4 is most of the time, and 5 is always. There is
a statistically significant increase in how frequently participants
thought about portion control and consumed low-fat foods. There
was no difference in mood, stress, sleep, and exercise (Table 3).
| |
Pre-intervention |
Post-intervention |
p-value |
| In the last 3 months, how often were you happy with your life? |
3.6 ± 0.9 |
3.6 ± 0.6 |
0.9 |
| In the last 3 months, how often were you stressed (or did you have had trouble relaxing)? |
2.9 ± 0.7 |
3.0 ± 0.9 |
0.8 |
| In the last 3 months, how often did you get enough sleep/wake up feeling refreshed? |
2.8 ± 0.8 |
3.0 ± 0.9 |
0.2 |
| In the last 3 months, how often did you think about the portion size of your snack or meal? |
2.6 ± 1.6 |
3.1 ± 1.0 |
0.02* |
| In the last 3 months, how often did you eat a low-fat diet or low cholesterol diet? |
1.9 ± 0.9 |
2.3 ± 0.9 |
0.03* |
| In the last 3 months, how often did you exercise enough to sweat, raise your beat, or make you sweat for more than 20 minutes? |
3.6 ± 1.4 |
3.8 ± 1.2 |
0.3 |
Table 3: ECHOS Phase 1: Behavioral health changes.
Phase 2
Pre-intervention results: Prior to the intervention, participants
reported that, on average, they were “unsure” to “somewhat
knowledgeable” about healthy sleep habits (3.65 ± 0.7) and the
impact of sleep on heart health (3.38 ± 0.92). In the 3 months
prior to the intervention, patients averaged 7.4 ± 0.9 hours.
We noted a moderate negative correlation (r=-0.55) [p<0.005]
between stress level and average hours of sleep. The average
pre-intervention MOS Sleep Problem Index (SPI) was 8.3 (out
of a maximum possible score of 15), indicating considerable
sleep disturbances. There was a moderate positive correlation
(r=0.52) [p=0.005] between stress level and sleep problem index.
Participants stated they were “unsure/slightly motivated” to get
enough sleep.
Post-Intervention Results: After the ECHOS phase 3 intervention
there was no significant difference in knowledge about healthy
sleep habits [p=0.08] or knowledge about the impact of sleep
on heart health [p=0.1] (Table 4). There was also no significant
change in motivation to improve sleep habits [p=0.5] (Table
4). There was a statistically significant increase in average total
quantity of sleep [p=0.003] and a decrease in average individual
sleep problems index score [p<0.005] (Tables 4 and 5).
| |
Pre-intervention |
Post-intervention |
p-value |
| Where do you rank yourself about your knowledge on healthy sleep habits? |
3.7 ± 0.7 |
3.5 ± 1.2 |
0.08 |
| Where do you rank yourself about your knowledge on the impact of sleep on your heart and overall health? |
3.4 ± 0.9 |
3.6 ± 1.2 |
0.6 |
| How motivated are you to get more/enough sleep? |
3.5 ± 1.0 |
3.7 ± 1.1 |
0.5 |
| Average quantity of sleep per night |
7.4 ± 0.9 |
7.8 ± 0.9 |
0.003* |
| Sleep Problem Index Score |
8.3 ± 2.0 |
7.0 ± 1.7 |
<0.005* |
Table 4: EECHOS Phase 2 results.
| |
Pre-Intervention |
Post-Intervention |
P-value |
| Sleep disturbance |
2.4 ± 0.8 |
2.0 ± 0.7 |
0.04* |
| Somnolence |
2.8 ± 0.8 |
2.3 ± 0.6 |
0.002* |
| Sleep adequacy |
3.2 ± 0.9 |
2.7 ± 0.8 |
0.005* |
Table 5: ECHOS Phase 2: Average individual change in Sleep Problem
Index Score (by domains).
There was no significant difference in knowledge about healthy
sleep habits [p=0.08] or knowledge about the impact of sleep on
heart health [p=0.1] (Table 4). There was no significant change in
motivation to improve sleep habits [p=0.5] (Table 4). There was a
statistically significant increase in average total quantity of sleep
[p=0.003] and a decrease in average individual sleep problems
index score [p<0.005].
Summing the scores across these three domains generates
the Medical Outcomes Study (MOS) Sleep Scale-Revised Sleep
Problems Index (SPI). Higher scores indicate more sleep problems
overall. A six-item questionnaire assessed three domains or
dimensions of sleep over the past 4 weeks. Respondents self-
reported how often they experienced the “sleep problem”
specified in the item using 5-point scales ranging from “none of
the time” to “all of the time.” Sleep disturbance included three
items: subjective feeling that sleep was not quiet/restful, trouble
falling asleep, and awakening during sleep time, and having
trouble falling asleep again. Somnolence referred to feeling
drowsy during the day and how common it was for them to take
daytime naps. Finally, adequacy was defined by the item about
“waking up feeling unrested.”
Phase 3
Pre-intervention Results: Building on our previous phases, the
LHQ-B was administered to assess various lifestyle behaviours
of participants. Higher scores on the LHQ-B suggest stronger
adoption of healthy patterns of behaviour for each particular
lifestyle domain, while lower scores represent less optimal,
health-compromising behaviour. There was a predominance of
female participants in this phase (n=125) compared to males
(n=28). Females tended to have higher scores in all of the domains
except psychological and physical health (Table 6).
| |
Male (n=28) |
Female (n=125) |
| Domains |
Pre |
Post |
P-value |
Pre |
Post |
P-value |
| Physical Activity |
20.4 |
19.9 |
0.4 |
17.7 |
18.5 |
0.09 |
| Psychological health |
26.7 |
26.2 |
0.3 |
23.7 |
24.7 |
0.06 |
| Substance Use |
34.2 |
36 |
0.1 |
35.7 |
36.3 |
0.1 |
| Nutrition |
11.4 |
11.8 |
0.3 |
11.8 |
12.6 |
0.1 |
| Social Concern |
19.8 |
20 |
0.4 |
20.7 |
20.1 |
0.04* |
| Sense of Purpose |
11.5 |
11.3 |
0.4 |
11.8 |
10.9 |
0.004* |
Table 6: ECHOS Phase 3: Lifestyle and Health Questionnaire-Brief
(LHQ-B) results.
Post-intervention Results: While there tended to be a statistically
significant change on individual questions within each lifestyle
domain between pre- and post-surveys, the aggregate score of
each domain was less sensitive to significant change. Of note,
psychological health, one of the domains suggestive of stress
levels, showed four significant sub-domain changes for females
and 1 for males from pre- to post-responses (Table 7) [6]. On the
whole, female scores tended to increase, suggesting improved
lifestyle over the course of study. In particular, females showed
scores significantly lower on the social concern (p=0.04) and
sense of purpose (p=0.004) domains from pre- to post-surveys.
For males, there were no statistically significant changes in any of
the six lifestyle domain scores (Tables 6 and 7).
| Sub-Domain Statements |
Male (n=28) |
Female (n=25) |
| Pre |
Post |
P-value |
Pre |
Post |
P-value |
| I am able to manage the stress in my life. |
3.9 |
3.7 |
0.09 |
3.2 |
3.5 |
0.003* |
| I am able to relax and unwind. |
4 |
4 |
0.4 |
3.6 |
3.6 |
0.3 |
| I am hopeful about the future. |
4.2 |
3.9 |
0.08 |
3.8 |
3.8 |
0.4 |
| I have clear direction in life. |
3.8 |
3.8 |
0.5 |
3.2 |
3.4 |
0.04* |
| I am able to concentrate on my work at school or on the job. |
3.9 |
3.9 |
0.3 |
3.6 |
3.7 |
0.1 |
| I get at least 7-8 hours of sleep at night and wake up feeling rested and refreshed. |
2.9 |
3.1 |
0.02* |
2.8 |
3.1 |
0.004* |
| I am able to assert myself in a responsible way and not allow others to take advantage of me. |
3.9 |
3.9 |
0.5 |
3.6 |
3.8 |
0.04* |
Table 7: ECHOS Phase 3: Changes for psychological health domain in
males and females.
The Lifestyle and Habits Questionnaire-Brief (LHQ-B) 6
assesses lifestyle behaviours and attitudes in young adults 18-
25. A modified LHQ-B with six of eight original domains was
adapted for pre- and post-surveys, including physical activity,
psychological health, substance use, nutrition, social concern,
and sense of purpose. According to the authors, the LHQ-B
domains of psychological health and social concern were the
top two domains that predicted stress levels. The study team was interested in sex differences in response to the intervention,
however, our sample did not allow for this. Females did; however,
tend to have higher relative scores in all of the domains except
psychological and physical health.
While there tended to be a statistically significant change on
individual questions within each lifestyle domain between pre
and post-surveys, the aggregate score of each domain was less
sensitive to significant change. Psychological health, one of
the domains suggestive of stress levels 6, which was the main
outcome of interest to the study team in phase 3, showed four
significant sub-domain changes for females and one for males
from pre- to post-responses.
Satisfaction with the text-messaging intervention
Phase 1: Participants shared what they learned from ECHOS
with family and friends some of the time (2.18 ± 0.13). A
majority (80%) were satisfied with the weekly text messages,
but the remaining 20% preferred more than one text-message a week. Text messages were the appropriate length for 92% of
participants. 94% would recommend the intervention to others.
Phase 2: 67% of participants liked receiving text messages every
other day during the month-long study while 33% would have
preferred to receive messages less frequently. 79% felt that the
texts were an appropriate length while 21% felt the texts were
too long. 60% read the majority of texts, but most participants
(71%) rarely or never attempted to interact with the text
messages by replying or clicking on a link to a resource provided.
The open-ended responses suggested that it was not necessarily
the way the texts were written, but rather that the participants
lacked a sense of accountability or motivation to engage with
the intervention and change their behaviours, “I think people
might be more motivated to change their sleep habits if this was
a ‘challenge’ system along with the facts provided.” 90% would
recommend the intervention to others.
Phase 3: Most participants “strongly agreed/agreed” that the
messages: increased their knowledge on how to live a heart-
healthy lifestyle (80%), were relevant to them (86%), increased
their awareness about their health (86%), and liked receiving the
messages (82%). Many participants expressed similar sentiments
as seen in the following example, “I started taking a bit more
control on relieving myself from stress.”
Discussion
This intervention focused on providing heart-healthy education
to adolescents and young adults using mobile health technology.
With the use of text messages, ECHOS brought cardiovascular
disease prevention to the fingertips of an otherwise difficult
to engage group, similar to previously reported interventions
employing text messaging or “nudge theory” [29-31].
ECHOS received positive feedback from participants, and high
satisfaction suggesting high acceptance of the use of digital
health and media among adolescents and young adults.
ECHOS demonstrated a modest increase in knowledge about
heart disease prevention. We observed changes consistent
with steps toward a heart-healthy lifestyle. While these were
encouraging findings, without any control group, there are many
possible confounding factors and threats to the internal validity
of the study. For example, phase 2 was conducted in summer
months, in which young people are less likely to have school and
work obligations governing sleep practices.
There was no significant difference in nutrition knowledge, a sense
of happiness, or exercise. There are several possible explanations
for the lack of significant differences. First, participants’ baseline
ratings for health knowledge were relatively high suggesting a
potential ceiling effect. Second, the intervention intensity and
length may not have been sufficient to detect a difference in
outcomes of interest. Another limitation is that our use of non-
probability, convenience sampling may mean that our cohorts
were not representative of general youth behaviour and health
literacy. Future research should include greater heterogeneity of
participants, including more male participants (our sample sizes
were too small to accurately assess sex differences). Given the wide access to mobile devices across different ages, races, and
socio-economic statuses, it is likely that this type of intervention
would produce similar findings. However, it is important to reach
underserved populations, in which the risk of chronic disease is
even greater.
While this mobile health intervention allowed participants
to occasionally reply to a text to receive another automated
message with more information, our platform could not respond
to individuals directly. This could certainly have affected the
participants’ motivation, value, and perception of the intervention.
More tailored and interactive texting may increase self-efficacy
and response efficacy in future interventions. Insufficient real-
time feedback for participants may represent a lost opportunity
to facilitate self-guided behaviour modification. Additionally, the
use of devices and interventions designed to share behavioural
data with both patients and healthcare professionals could
provide even more valuable insight in between clinic visits, for
example. Future research could focus on further evaluation of
text message attributes (e.g., tone of the messages), expanding
to tracking clinical or physiological measures (e.g., weight or
pulse), and the use of the resources provided in the texts.
Conclusion
The ECHOS study is one of many examples that demonstrate the
potential of constantly evolving personalized, digital technology
to support healthy lifestyle management and early prevention
of chronic illness, including cardiovascular disease. Our three
pilot trials of ECHOS can help shape and inform future full-scale
studies in these arenas. Our findings indicate it is feasible and
scalable for participants to use and track cardiovascular health-
related data and lifestyle behaviour for at least 1-3 months via
a text-messaging intervention. Continued efforts are needed to
elucidate and eliminate barriers to awareness, education, and
implementation of preventive health behaviours.
As cell phones have become ubiquitous in our daily lives, text
messaging offers a quick and less daunting way to incorporate
and track many holistic health behaviours, big and small. This
makes improved health accessible regardless of where someone
is on their health journey, whether it is through learning, trying
something new, or changing up an old routine. It is a creative
approach for improving cardiovascular risk profiles in adolescents
and young adults, especially, but may also benefit all ages.
Conflict of Interest
“All authors have completed the Unified Competing Interest
form (available on request from the corresponding author) and
declare: no support from any organization for the submitted
work; no financial relationships with any organizations that might
have an interest in the submitted work in the previous 3 years;
no other relationships or activities that could appear to have
influenced the submitted work.” Grant funding for research but
no other competing interests.
Acknowledgements
Dr. Armen Arevian for allowing us to implement the study using
his Chorus app.
Dia Collins for her tireless support of our entire research team.
Garett Collins for vetting our text messages.
Vadim Osadchiy M.D. for his assistance with phase 1.
UCLA Internal Medicine Chiefs’ Summer Research Fellowship &
Zekun Feng M.D. for providing mentorship, consistent feedback,
and encouragement in phase 2.
UCLA Undergraduate Research Fellows Program for mentorship
and for generous financial support of the UCLA Wasserman
Scholarship, which made possible the gift cards in phase 3.
References
- Bucholz EM, Gooding HC, de Ferranti SD (2018) Awareness of cardiovascular risk factors in US young adults aged 18-39 years. Am J Prev Med 54:67-77.
- Fryar CD, Ostchega Y, Hales CM, Zhang G, Kruszon-Moran D (2017) Hypertension Prevalence and Control Among Adults: United States, 2015-2016.
- Gooding HC, Shay CM, Ning H, Gillman MW, Chiuve SE, et al. (2015) Optimal lifestyle components in young adulthood are associated with maintaining the ideal cardiovascular health profile into middle age. J Am Heart Assoc 4:e002048.
- Lawrence EM, Mollborn S, Hummer RA (2017) Health lifestyles across the transition to adulthood: Implications for health. Soc Sci Med 193: 23-32.
- Celermajer DS, Ayer JG (2006) Childhood risk factors for adult cardiovascular disease and primary prevention in childhood. Heart 92:1701-1706.
- Dinzeo TJ, Thayasivam U, Sledjeski EM (2014) The development of the Lifestyle and Habits Questionnaire-brief version: Relationship to quality of life and stress in college students. Prev Sci 15:103–114.
- World Health Organization (2005) Preventing chronic diseases: A vital investment.
- Grewen KM, Girdler SS, Amico J, Light KC (2005) Effects of partner support on resting oxytocin, cortisol, norepinephrine, and blood pressure before and after warm partner contact. Psychosom Med 67:531-538.
- Yoshikawa Y, Ohmaki E, Kawahata H, Maekawa Y, Ogihara T, et al. (2019) Beneficial effect of laughter therapy on physiological and psychological function in elders. Nurs Open 6:93-99.
- University Of Maryland Medical Center (2005) University of Maryland School of Medicine Study Shows Laughter Helps Blood Vessels Function Better.
- Ogechi I, Snook K, Davis BM, Hansen AR, Liu F, et al. (2016) Pet ownership and the risk of dying from cardiovascular disease among adults without major chronic medical conditions. High Blood Press Cardiovasc Prev 23:245-253.
- Mubanga M, Byberg L, Nowak C, Egenvall A, Magnusson PK, et al. (2017) Dog ownership and the risk of cardiovascular disease and death-a nationwide cohort study. Sci Rep 7:1-9.
- Narang I, Manlhiot C, Davies-Shaw J, Gibson D, Chahal N, et al. (2012) Sleep disturbance and cardiovascular risk in adolescents. CMAJ 184: E9130-E920.
- Fredriksen K, Rhodes J, Reddy R, Way N (2004) Sleepless in Chicago: Tracking the effects of adolescent sleep loss during the middle school years. Child Dev 75: 84-95.
- Van Der Werf YD, Altena E, Schoonheim MM, Sanz-Arigita EJ, Vis JC, et al. (2009) Sleep benefits subsequent hippocampal functioning. Nat Neurosci 12: 122-123.
- Feliciano EMC, Quante M, Rifas-Shiman SL, Redline S, Oken E, et al. (2018) Objective sleep characteristics and cardiometabolic health in young adolescents. Pediatrics 142:e20174085.
- Centers for Disease Control and Prevention. Short sleep duration among high school students: Youth risk behavior survey, United States, 2007-2013.
- Johnson HM, Warner RC, LaMantia JN, Bowers BJ (2016) “I have to live like I’m old.” Young adults’ perspectives on managing hypertension: A multi-center qualitative study. BMC Fam Pract 17: 1-9.
- Cole-Lewis H, Kershaw T (2010) Text messaging as a tool for behavior change in disease prevention and management. Epidemiol Rev 32: 56-69.
- Naughton F, Jamison J, Boase S, Sloan M, Gilbert H, et al. (2014) Randomized controlled trial to assess the short-term effectiveness of tailored web- and text-based facilitation of smoking cessation in primary care (iQuit in practice). Addiction 109: 1184-1193.
- Maddison R, Stewart R, Doughty R, Scott T, Kerr A, et al. (2018) Text4Heart II-improving medication adherence in people with heart disease: A study protocol for a randomized controlled trial. Trials 19: 1-10.
- Oosterveen E, Tzelepis F, Ashton L, Hutchesson MJ (2017) A systematic review of e-Health behavioral interventions targeting smoking, nutrition, alcohol, physical activity and/or obesity for young adults. Prev Med 99:197-206.
- Smith A (2011) Americans and text messaging. Pew Research Center: Internet. Science & Tech.
- Thaler R, Sunstein C (2009) Nudge: Improving Decisions About Health, Wealth, and Happiness. Penguin Books 1-312.
- Patel MS, Volpp KG, Asch DA (2018) Nudge units to improve the delivery of health care. N Engl J Med 378(3):214-216.
- Bell ML, Whitehead AL, Julious SA (2018) Guidance for using pilot studies to inform the design of intervention trials with continuous outcomes. J Clin Epidemiol 10: 153-157.
- Hays RD, Sherbourne CD, Mazel RM (1995) User's manual for the Medical Outcomes Study (MOS) core measures of health-related quality of life. Santa Monica: Rand Corporation.
- Yarlas AS, White MK, Smith KJ, Bjorner JB (2012) QU1 the development and validation of a revised version of the medical outcomes study sleep scale (MOS-Sleep-R). Value Health 15:A11.
- Markowitz JT, Cousineau T, Franko DL, Schultz AT, Trant M, et al. (2014) Text messaging intervention for teens and young adults with diabetes. J Diabetes Sci Technol 8:1029-1034.
- Gipson CS, Chilton JM, Dickerson SS, Alfred D, Haas BK (2019) Effects of a sleep hygiene text message intervention on sleep in college students. J Am Coll Health 67: 32-41.
- Glowacki EM, Kirtz S, Hughes Wagner J, Cance JD, Barrera D, et al. (2018) HealthyhornsTXT: A text-messaging program to promote college student health and wellness. Health Promot Pract 19: 844-855.