Keywords
Obesity; Paediatric; Resilience; Sleep; Screen Use; Overweight; Pre-Schoolers
Introduction
Childhood obesity remains one of the most prominent public health issues of our time, with 30% of New Zealand children aged 2-4 years classified as being overweight or obese [1]. Not only is obesity in early childhood associated with gastroenterological, endocrine, cardiovascular, orthopaedic, and respiratory issues, in addition to psychological outcomes such as low self-esteem, social isolation, and bullying [2], it is also a strong predictor of adult obesity [3,4] and an important early risk factor for considerable morbidity and mortality in adulthood [5].
Childhood overweight and obesity differ according to ethnicity and socioeconomic status (SES), with higher rates observed in Maori, the indigenous people of New Zealand (42.9%), Pacific (56.5%), and the most deprived families (42.3%) [3]. Children with higher rates of overweight and obesity appear disproportionately affected due to differences in exposure to almost all the known risk factors for childhood obesity [6,7], including disparities in the built environment leading to reduced opportunity for physical activity [8], the relatively low-cost of energy-dense, nutrient-poor foods [9], and high levels of stress and insecurity [10], which in turn are linked with health-related behaviours associated with a higher body mass index (BMI). Accordingly, it is recommended that the modifiable risk factors, such as consumption of fast foods or sugar-sweetened beverages, associated with disparities in childhood obesity should be reduced or prevented [11].
Yet, despite exposure to the obesogenic environment, a large proportion of at-risk children are still able to maintain a healthy bodyweight [12]. It has been argued that these children demonstrate bodyweight resilience [12], that is, despite exposure to adversity or vulnerability they are still able to obtain a positive outcome of a healthy bodyweight. In order to identify modifiable factors associated with bodyweight resilience, researchers have reasoned that we must establish how families facing adversity with healthy weight children differ in the way they construct their daily lives compared with families facing adversity with overweight children [13]. Such an approach assumes that families of resilient children are already engaging in effective solutions to preventing obesity that are actionable within their own community and family context [14].
By identifying characteristics associated with bodyweight resilience we may be able to provide families of children facing adversity with a pathway to health that is not only immediately actionable within their own family context, but also less likely to increase health disparities [14]. The purpose of this study was therefore to identify family-level factors associated with bodyweight resilience in a large cohort of New Zealand families.
Materials and Methods
Data and sample
Data for this study were taken from Growing Up in New Zealand (GUiNZ), a prospective cohort study that recruited 6846 mothers whose babies were due to be born between April 2009 and March 2010 [15]. The study design, recruitment process, and data collection methods have been described previously in detail [16]. Participants were drawn from the greater Auckland and Waikato regions to provide a socioeconomically and ethnically diverse sample, which has been demonstrated to be representative of the broader New Zealand birth population [16]. For the purpose of this analysis, we used data from the face-to-face interviews completed with the child’s caregiver, usually the mother, when the child was 9 months of age (wave 1; n=6476), 24 months of age (wave 2; 6327), and 54 months of age (wave 5; 6156; 90%), as well as telephone interviews conducted as Computer Assisted Telephone Interviews (CATI) when the child was 45 months of age (wave 4; n=6211). This analysis was conducted in a sub-group of 1367 children.
Children were included in the current analysis if 1) Their data was available at each of the four above data collection waves 2) They were classified as being at risk for overweight or obesity (definition provided below), and 3) Body Mass Index (BMI) data was available at 4.5 years. Logistic regression requires observations to be independent of each other, and including multiple births would violate this assumption. As such, for multiple births, only one twin or triplet was included.
Given that resilience is defined as a process through which positive outcomes are achieved in the context of risk or adversity [17], it is necessary to define ‘risk’ and a ‘positive outcome’.
Definition of risk: We assessed risk using the GUiNZ maternal vulnerability scale (Table 1) [16]. The twelve maternal risk factors included in the GUiNZ maternal vulnerability scale were selected according to previous use in international research to define markers of disadvantage and what makes a child vulnerable for poor outcomes across the life course [18]. Each of the twelve maternal risk factors was dichotomised with a score of 0 or 1, according to whether risk was experienced or not.
| Risk Factor |
Definition |
| Maternal depression |
EPDS = 12 |
| Maternal physical wellbeing |
Poor/fair |
| Maternal smoking |
Continuing to smoke after 1st trimester of pregnancy or continuing to smoke regularly/every day |
| Maternal age |
Aged less than 20 years |
| Relationship status |
Single/no current partner |
| Maternal education |
No secondary school qualifications |
| Financial stress |
Reporting “highly stressful” money problems |
| Deprivation area |
Living in areas situated within the two most deprived deciles |
| Unemployment |
Mother not on leave, actively seeking work but not currently working |
| Tenure-public rental |
Living in social housing |
| Income tested benefit |
In receipt of an income tested government benefit |
| Overcrowding |
Having 2 or more persons per bedroom |
| Note: EPDS=Edinburgh Postnatal Depression Scale |
Table 1: Definitions of included risk factors.
Previous GUiNZ reports have classified vulnerability at any point in time into three sub-groups: low (no exposure to vulnerability risk factors), medium (exposure to 1-3 factors), or high (exposure to 4 or more factors) [19,20]. For the purpose of this resiliency to obesity analysis we wanted to dichotomise our measure of risk into two groups: (1) low risk, and (2) at risk. One option was to create the at-risk group by combining the medium- and high-risk groups, using the definition from previous reports. This would mean the at-risk group would include any child demonstrating at least one vulnerability risk factor; however, only including one risk factor has been identified as a limitation of previous resiliency research [21] and further, a number of the maternal stress measures included in the generic GUiNZ maternal vulnerability scale have not been directly associated with childhood obesity [22]. As such the decision was made to exclude children only demonstrating one vulnerability factor from the at-risk group in order to provide a more robust measure of vulnerability for the specific outcome related to obesity.
Nevertheless, we did not want to exclude all children demonstrating moderate risk, as this would have reduced the sample size of the at-risk group substantially, and also meant that the findings would only be relevant to a small, highly vulnerable group of children. As such, the pragmatic decision to dichotomise risk into the following two groups was made: (1) Low risk, defined as having no exposure to vulnerability risk factors, and at risk, defined as having exposure to at least two vulnerability risk factors.
Researchers argue that alone exposure to vulnerability factors is not an adequate definition of at risk, and that there must also be the demonstration of continuous or chronic exposure to these vulnerability factors [23]. According to a previous GUiNZ analysis [22], exposure to maternal stressors during the pre- and postnatal period were significantly and positively associated with child BMI at 54 months, with cumulative or chronic maternal stress having the greatest effect on child BMI, when compared with stress experienced at only one time point [22]. These findings corroborate research that has shown that children exposed to chronic poverty have worse outcomes compared with children exposed to intermittent or episodic poverty [24]. As such, we classified children as being at risk for overweight and obesity if they demonstrated cumulative vulnerability, defined as having a mother with at least two vulnerability risk factors at both 9 months and 24 months. Low-risk children were defined as those with mothers with no maternal risk factors at both time points. Children with only one vulnerability risk factor or who had nonconsistent risk, defined as those whose risk changed categories between the two time points, were excluded from the analysis.
Definition of a positive outcome: We defined a positive outcome as not being overweight or obese at age 4 years. BMI was calculated using weight and height measures from the 4.5-year data collection wave, and standardised to z-score using the World Health Organization growth standards [25]. A classification for overweight or obese was based on the Extended International Obesity TaskForce BMI cut-off values [26].
Resiliency: A child was classified as being resilient if they were considered to be at risk for overweight and obesity but with a positive outcome (i.e. not overweight or obese; n=1054) and non-resilient if they were considered to be at risk for overweight and obesity with a negative outcome (i.e. overweight or obese; n=313). Given that resilience requires exposure to risk, only those children classified as being at risk were included in this analysis (n=1367) (Figure 1), therefore those children with low cumulative risk and a positive outcome (n=1829), and low cumulative risk and a negative outcome (n=129) were excluded.
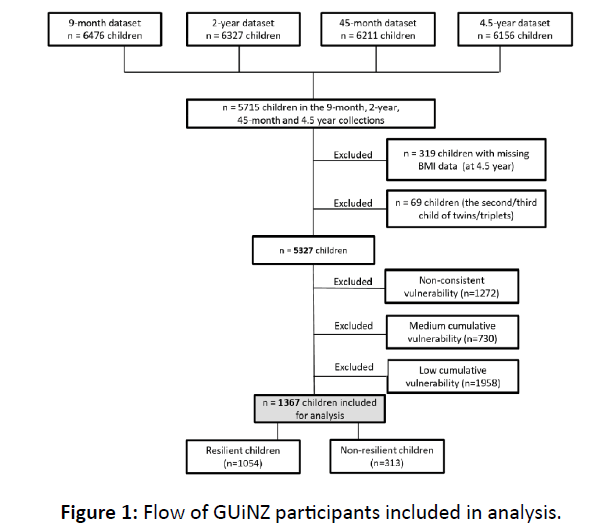
Figure 1: Flow of GUiNZ participants included in analysis.
Protective factors: Protective factor variables were collected at the 9-month, 24-month, and 45-month GUiNZ data waves. We selected potential protective factors for inclusion in the model according to literature demonstrating components of family resiliency that might be related to childhood overweight [13], and factors that have been linked with childhood obesity but that are not directly related to energy balance, including parenting and parenting factors [27-29], presence of family routines [30], child sleep [31-33], screen use [34], and the family mealtime environment [35-38]. The decision was made to exclude traditional weight-management approaches directly related to energy balance for two reasons: (1) Traditional approaches that focus directly on weight-related behaviours may be less acceptable to families of young children [39], and (2) the promotion of traditional weight-related behaviours in young children have been associated with an increased risk for overweight and obesity compared with non-traditional weightrelated behaviours in young New Zealand children [40]. Protective factors investigated are presented in Table 2.
| Time point |
Protective factor |
Domain |
How assessed |
| 9 months |
Frequency that the TV is turned on in the same room as child, whether or not they are watching |
Screen use |
Single item; “How often is the TV turned on in the same room with your baby [babies], whether or not your baby is [babies are] watching?” |
| 9 months |
Parental self-efficacy score |
Parenting |
Single score; 11 items derived from ‘What being the parent of a baby is like (WPL-R)’ questionnaire [48] |
| 9 months |
Satisfaction with help from partner |
Family factors |
Single item; “How satisfied are you with the help you get from your partner?” |
| 9 months |
Satisfaction with help from family |
Family factors |
Single item; “How satisfied are you with the help you get from your family?” |
| 2 years |
Maternal separation anxiety |
Parenting |
Single item; “How often does leaving child with other people upset you no matter how well you know them?” |
| 2 years |
Parental enjoyment score |
Parenting |
Composite score*; 4 items |
| 45 months |
Total night time sleep |
Sleep |
Single item; “On average, how much time does child spend asleep at night in total?” |
| 45 months |
Total daytime sleep (hours/day) |
Sleep |
Single item; “On average, how much time does child spend asleep during the day?” |
| 45 months |
Frequency of night-time wakening |
Sleep |
Single item; “On average how many times does wake at night?” |
| 45 months |
Mealtimes are enjoyable |
Family mealtime environment |
Single item; “Mealtimes are enjoyable for everyone” |
| 45 months |
Mealtimes are a rush |
Family mealtime environment |
Single item; “Mealtimes are a rush” |
| 45 months |
Mealtimes give the family time to talk to each other |
Family mealtime environment |
Single item; “Mealtimes give us time to talk to each other” |
| 45 months |
Frequency of TV on during child’s mealtimes |
Family mealtime environment |
Single item; “How often is the TV on in the same room when your child is eating a meal?” |
| 45 months |
Engagement in routines score (composite score*) |
Family routines** |
Composite score*; 7 items |
| 9 months and 2 years*** |
Parent-child relationship score at 9-month and 2-year |
Parenting |
Composite score*; 12 items |
| 2 years and 45 months*** |
Total (direct and indirect) screen exposure at 2-year and 45-month (hours/day) |
Screens |
Composite score*; 3 items |
| Note": *Responses for each item were dichotomised and then summed. **Family routines investigated included frequency that the child eats breakfast, frequency of family meals, frequency that TV is on during meals, frequency that child brushes teeth, sleep (night and daytime duration), whether the child goes to bed at a similar time each night. *** When outcomes were assessed at multiple time points, the average of the scores was used in the analysis. |
Table 2: Protective factors investigated in univariate analysis.
Data analysis
Descriptive statistics were summarized separately for the groups of children, using median with interquartile range (IQR) for continuous and numbers with percentages for categorical data respectively. Two high adversity groups (i.e. resilient vs. nonresilient) were tested using logistic regression analysis to examine the potential protective factors distinguishing resilient children from non-resilient children. Univariate logistic regressions were first conducted using each of the protective factors for inclusion in the multivariate logistic regression model. The multivariate model included significant protective factors with a more liberal p-value of 0.15 in the univariate model [41], as well as those that were identified as potential confounders regardless of statistical significance. For multivariate logistic regression models, control variables including child’s gender, gestational age in weeks, and birth weight. M and maternal relationship status, employment status, ethnicity, education level, and pre-pregnancy BMI, were also added to the models. These factors were selected due to previous research demonstrating them to be associated with child health-related behaviours and/or weight status.
Multivariate model results were presented as odds ratios (OR) with the corresponding 95% confidence intervals (95% CI) and p-values. A Two-tailed p-value <0.05 considered statistically significant. Multicollinearity among protective factors was assessed with (i) Pearson’s correlation coefficient for continuous variables, (ii) Spearman’s rank correlation coefficient or Chi- Square test for categorical variables and (iii) t-test or one-way analysis of variance (ANOVA) for a continuous and a categorical variable. On the basis of the results of these tests, the potential predictors showed no problematic collinearity. Missing data on individual protective factors were not imputed and multivariate analyses were performed on complete data only. ‘Partner satisfaction with help’ was a protective factor that contributed the most to the missing data (n=290 for resilient children and n=82 for non-resilient). This factor was considered as important and not simply excluded from the analysis. All statistical analyses were performed using SAS software version 9.4 (SAS Institute, Cary, NC, USA).
Results
Control variables for resilient (n=1054) and non-resilient (n=313) children are reported in Table 3.
| |
Resilient (n=1054) |
Non-resilient (n=313) |
P-value |
| Child Variables (n, %) |
| Gender |
| Boy |
537 (50.9) |
181 (57.8) |
0.033 |
| Girl (ref) |
517 (49.1) |
132 (42.2) |
| Gestational age in weeks |
| Pre-term (<37 weeks) |
82 (7.8) |
14 (4.5) |
0.128 |
| Term (37-41 weeks; ref) |
944 (89.9) |
289 (92.6) |
| Post-term (>41 weeks) |
25 (2.4) |
9 (2.9) |
| Missing |
3 (-) |
1 (-) |
| Birthweight |
| Low birth weight (<2500 g) |
69 (6.5) |
9 (2.9) |
<0.0001 |
| Appropriate birth weight (2500-4000 g; ref) |
846 (80.3) |
224 (71.6) |
| High birth weight (>4000 g) |
139 (13.2) |
80 (25.6) |
| Caregiver Variables (n, %) |
| Relationship status* |
| Partner (ref) |
610 (58.2) |
196 (62.8) |
0.146 |
| No partner |
438 (41.8) |
116 (37.2) |
| Missing |
6 (-) |
1 (-) |
| Employment status |
| Employed (ref) |
298 (28.4) |
95 (30.4) |
0.772 |
| Unemployed |
460 (43.8) |
133 (42.6) |
| Change in employment status** |
293 (27.9) |
84 (26.9) |
| Missing |
3 (-) |
1 (-) |
| Self-prioritised ethnicity |
| European (ref) |
366 (34.9) |
77 (24.7) |
<0.0001 |
| Maori |
273 (26.0) |
91 (29.2) |
| Pacific |
271 (25.8) |
128 (41.0) |
| Asian |
108 (10.3) |
11 (3.5) |
| MELAA, Other or New Zealander |
32 (3.0) |
5 (1.6) |
| Missing |
4 (-) |
1 (-) |
| Education level |
| No secondary school qualification |
210 (20.0) |
56 (18.1) |
0.042 |
| Secondary school/NCEA 1-4 |
321 (30.6) |
108 (34.8) |
| Diploma/Trade certificate/NCEA 5-6 (ref) |
371 (35.4) |
120 (38.7) |
| Bachelor’s degree/ Higher degree |
146 (13.9) |
26 (8.4) |
| Missing |
6 (-) |
3 (-) |
| Maternal BMI before pregnancy (WHO standard) |
| Underweight/Normal (<25 kg/m2) |
392 (48.1) |
49 (23.0) |
<.0001 |
| Overweight (25-30 kg/m2; ref) |
200 (24.5) |
50 (23.5) |
| Obese (>30 kg/m2) |
223 (27.4) |
114 (53.5) |
| Missing |
239 (-) |
100 (-) |
| Ref=reference group. *Information on partner status was obtained from the 9-month, 2-year and 4.5-year interviews. It was defined as “no” if the mothers had no partners during the study period and “yes” if they had a partner at least one of the time points. **Information on employment status was obtained from the 2-year and 4.5-year interviews. |
Table 3: Demographic and baseline variables for children considered at risk for overweight/obesity.
Univariate findings
The odds of a child being classified as resilient were first examined for each of the protective factors individually (data are not shown). The unadjusted model showed that less maternal separation anxiety was associated with significantly greater resilience in children (OR=1.42, p=0.0069). Children were also more likely to be categorised as resilient rather than non-resilient if they had less frequent TV exposure during mealtimes, or longer nighttime sleep duration (OR=1.24, p<0.0001), with this association remaining after adjusting for possible confounders. Alternatively, resilience was inversely associated with mealtimes being rushed (OR=0.54, p=0.0011). Further, children with greater direct and indirect screen exposure (OR=0.89, p=0.0436), or from families with lower parental self-efficacy (OR=0.97, p=0.0195) and family satisfaction (OR=0.84, p=0.0004) had a lower likelihood of being resilient.
Multivariate findings
Findings from the multivariate analyses are presented in Table 4. Only those protective factors that were statistically significant at univariate analyses, defined as having a p-value of ≤ 0.15, or those considered to have scientific relevance (e.g. TV on in the same room as the child) were included. As mentioned in the analysis section, each model was also controlled for predefined confounders. Child’s birth weight and maternal pre-pregnancy BMI had a significant effect on the dependent variable (being a resilient child).
| Variable |
Time Point |
P-value |
Adjusted odds ratio (95% CI) |
| How often is the TV turned on in the same room with your baby, whether or not your baby is watching? |
9 months |
0.567 |
0.869 (0.536-1.407) |
| Seldom or never/ Once a week/ Several times a week |
| Once a day/ Several times a day (ref) |
| Parental self-efficacy score |
9 months |
0.59 |
0.990 (0.953-1.028) |
| Satisfaction with family help |
9 months |
0.061 |
0.882 (0.774-1.006) |
| How often does leaving child with other people upset you no matter how well you know them?* |
2 years |
0.052 |
1.410 (0.998-1.992) |
| Never/ Rarely/ Occasionally |
| Often/ Very often (ref) |
| Mealtimes are a rush? |
45 months |
0.438 |
0.804 (0.462-1.397) |
| Never/ Rarely/ Occasionally (ref) |
| Quite often/ Mostly |
| Mealtimes give your family time to talk to each other? |
45 months |
0.067 |
1.517 (0.971-2.371) |
| Never/ Occasionally |
| Quite often/ Mostly (ref) |
| How often is the TV on in the same room when child is eating a meal? |
45 months |
0.176 |
1.301 (0.888-1.905) |
| Never/ Almost never |
| Sometimes/ Almost always/ Always (ref) |
| Total night time sleep, hours/day |
45 months |
0.0004 |
1.237 (1.099-1.392) |
| Total (direct and indirect) screen exposure, hours/day |
2 years & 45 months |
0.165 |
1.149 (0.944-1.398) |
| Note: *Maternal separation anxiety: P-values in bold represent significant associations (p <0.05) i.e., the 95% confidence intervals (CI) do not cross 1. The multivariate model was adjusted for cohort child gender, gestational age, birth weight and maternal characteristics (partner status, employment, self-prioritised ethnicity, education level, BMI in kg/m2). Resilient children i.e. those considered to be at-risk but demonstrating a healthy bodyweight, were the reference category in this analysis. |
Table 4: Multivariate model of vulnerability in resilient children vs. non-resilient children.
Resilient (n=750) vs. Non-resilient (n=197) children. Only one protective factor, night-time sleep duration, was significantly associated with an increase in the odds of being resilient (p=0.0004). A 1-hour increase in the night-time sleep duration increased odds of being in the resilient group by 24% (OR=1.24, 95% CI=1.10-1.39). No significant effects were shown for other protective factors (p>0.05).
Discussion
This study aimed to identify characteristics of families with children demonstrating bodyweight resilience. To our knowledge, this is the first study that has investigated the construct of bodyweight resilience in pre-school children. According to our analysis, total night time sleep duration was protective against childhood overweight and obesity in vulnerable children. Specifically, a 1-hour increase in night time sleep duration was found to increase the odds of being a healthy weight in children classified as being at-risk for overweight and obesity by 24%. No other factors were found to be associated with bodyweight resilience in the multivariate analysis.
For the present analysis we used data from a subset of children involved in New Zealand’s largest longitudinal cohort study, which has been shown to align with the birth characteristics of all New Zealand births over the period 2007-2011 [15]. Other strengths include our definition of resiliency, which included both an objective measure of a positive outcome and a cumulative measure of risk that has been shown to be significantly associated with increased BMI in this population [22]. Despite these strengths, we also identified a number of limitations.
As with many longitudinal studies, the study data contained a considerable amount of missing values on protective factors. These missing data were not imputed because they did not occur at random and it may have introduced more bias when using imputation methods than complete case analysis. Thus, multivariate analyses were conducted on complete data (i.e. nonmissing data) only. Another limitation was that twins and triplets were included in our analysis, which may represent a source of confounding, given growth trajectories may differ in the early years between singleton and multiple births. Additionally, the protective factors we used relied on self-report and therefore were at risk of social desirability and recall bias. Further, these factors had to be drawn from questionnaires that were not specifically designed for the purpose of this resiliency analysis. In addition, our definition of risk was based on the GUiNZ maternal vulnerability scale [16]. While a previous analysis demonstrated an association between maternal stress and BMI in this dataset, this previous analysis used a derived version of the scale (9/12 of the vulnerability measures), which specifically looked at the stressors shown in previous research to be associated with BMI [22]. Further, when defining risk, the research team made a pragmatic decision to use two vulnerability factors as a cut-off for defining at risk. Yet it is possible that using a different cut-off, in particular four vulnerability factors as used in previous reports, would yield a different result with respect to vulnerability factors. However, defining at risk as having four vulnerability factors at both time points reduced the sample size in the resilient group considerably, and we argue that this may have impacted on our ability to translate the findings beyond a small group of very highrisk children. Finally, while night-time sleep was associated with resiliency, we cannot say sleep causes vulnerable children to be a healthy weight. In fact, the relationship between sleep and bodyweight resilience is likely to be complex and the result of a number of direct and indirect pathways.
Our primary finding, that night time sleep duration is protective of overweight and obesity in vulnerable children, aligns with findings from previous studies [31,33,39,40,42]. According to a meta-analysis investigating the association between childhood obesity and sleep duration, short sleep duration was found to be associated with an increased risk of obesity in childhood in diverse populations and therefore was identified as an important factor for future obesity prevention strategies [43]. Yet while sleep has consistently been linked with a reduced risk of obesity, the role of sleep as a pathway to bodyweight resilience is novel. In contrast, a recent New Zealand study that investigated bodyweight resilience in children did not identify sleep duration as protective against overweight and obesity in at-risk children [14]. Instead, the study found engagement in regular family meals, the presence of food-related rules at home, and limiting screen time as being protective. However, the study differed in a number of important ways from the current analysis: it was conducted in adolescent children, the sample size was considerably smaller (n=30 families), it used an appreciative inquiry perspective to investigate the construct of bodyweight resilience, and it used a different measure of risk, namely low SES Pacific children.
The findings from this previous study align more with the results from our univariate analysis, which identified a number of other characteristics of families that appeared to be associated with bodyweight resilience, including lower direct and indirect screen time, TV less likely to be on in the same room as the child throughout the day and during meals, and a higher quality of family meals, including mealtimes less likely to feel rushed and mealtime offering an opportunity for the family to talk. Interestingly, when we ran the multivariate analysis these factors were no longer significant, suggesting that while important, they were likely to be related to night time sleep duration. These other variables may actually represent the broader construct of family organisation, which has also been linked with sleep duration. For example, it has been shown that children are more likely to have age-appropriate sleep patterns in the presence of household rules and regular routines around sleep. A cross-sectional study of US children aged 6-17 years found that well-established rules surrounding sleep hygiene were protective of sufficient sleep quantity and quality [44]. Alternatively, a chaotic home environment has been linked with dysregulated sleep patterns in families with young infants [45]. As such, the relationship between family organisation and sleep outcomes may be partly explained by findings that, in pre-school children, sleep timing moderates the relationship between night time sleep duration and BMI [46]. Taken together, the findings from previous research, in addition to both the univariate and multivariate analyses conducted here, suggest that while sleep is associated with bodyweight resilience, this may actually reflect greater organisation in the home environment, which in turn is supportive of sleep. As such, just promoting adequate night time sleep in pre-schoolers may not be sufficient, there may also be a need to reduce household chaos and promote greater family organisation
Future directions include elucidating whether it is sleep alone or sleep in the broader context of family organisation those results in bodyweight resilience, and whether similar findings would be found if different measures of risk were used. In particular, although the decision was made to use a measure of risk at two time points, future analysis may investigate whether findings differ when children with changing risk profiles are included in the analysis. Preliminary evidence suggests that targeting sleep in low income, racial/ethnic minority families has potential to reduce BMI in pre-school children [47] and future studies should attempt to replicate this in different populations with different definitions of risk. Finally, it is also important to establish how best to improve long-term sleep outcomes in pre-schoolers in a way that is developmentally safe, culturally appropriate, and protective of the parent-child relationship.
Conclusion
The current analysis demonstrates the importance of night time sleep duration specifically, and family organisation more generally, in promoting bodyweight resilience in children exposed to a cumulative measure of risk.
Funding
Samantha Marsh was supported by a New Zealand Lotteries Fellowship grant, a Heart Foundation Postdoctoral Fellowship, and internal funding from the University of Auckland, New Zealand
Acknowledgements
All authors contributed to the design and writing of the paper and had final approval of the submitted and published version. Samantha Marsh drafted the manuscript. Yeunhyang Catherine Choi performed the analysis. Samantha Marsh, Yeunhyang Catherine Choi, and Susan Morton contributed to the analysis plan, reviewed initial outputs, and contributed to data interpretation. S. M. was involved with study design and direction, funding, ethics, and overview. Samantha Marsh was supported by a New Zealand Lotteries Fellowship grant, a Heart Foundation Postdoctoral Fellowship, and internal funding from the University of Auckland.
Ethical Consideration
Ethical approval for GUiNZ was obtained from the Ministry of Health Northern Y Regional Ethics Committee (NTY/08/06/055).
Conflicts of Interest
None reported.
References
- www.moh.govt.nz/notebook/nbbooks.nsf/0/997AF4E3AAE9A767CC257F4C007DDD84/$file/annual-update-key-results-nzhs-2013-14-dec14.pdf
- Dietz WH (1998) Health consequences of obesity in youth: Childhood predictors of adult disease. Pediatrics 101:518-25.
- De Kroon ML, Renders CM, Van Wouwe JP, Van Buuren S, Hirasing RA (2010) The Terneuzen birth cohort: BMI changes between 2 and 6 years correlate strongest with adult overweight. PLoS One 5:e9155.
- Singh AS, Mulder C, Twisk JW, van Mechelen W, Chinapaw MJ (2008) Tracking of childhood overweight into adulthood: A systematic review of the literature. Obes Rev 9:474-88.
- Freedman DS, Dietz WH, Srinivasan SR, Berenson GS (1999) The relation of overweight to cardiovascular risk factors among children and adolescents: The Bogalusa Heart Study. Pediatrics 103:1175-82.
- Taveras EM, Gillman MW, Kleinman K, Rich-Edwards JW, Rifas-Shiman SL (2010) Racial/ethnic differences in early-life risk factors for childhood obesity. Pediatrics 125:686-95.
- Speirs KE, Hayes JT, Musaad S, VanBrackle A, Sigman-Grant M, et al. (2016) Is family sense of coherence a protective factor against the obesogenic environment? Appetite 99:268-76.
- Gordon-Larsen P, Nelson MC, Page P, Popkin BM, et al. (2006) Inequality in the built environment underlies key health disparities in physical activity and obesity. Pediatrics 117:417-24.
- Drewnowski A (2010) The cost of US foods as related to their nutritive value. Am J Clin Nutr 92:1181-8.
- Evans GW, Gonnella C, Marcynyszyn LA, Gentile L, Salpekar N (2005) The role of chaos in poverty and children's socioemotional adjustment. Psychol Sci 16:560-5.
- Taveras EM, Gillman MW, Kleinman KP, Rich-Edwards JW, Rifas-Shiman SL (2013) Reducing racial/ethnic disparities in childhood obesity: The role of early life risk factors. JAMA Pediatr 167:731-8.
- Ball K, Crawford D (2006) Socio-economic factors in obesity: A case of slim chance in a fat world? Asia Pac J Clin Nutr 15:15-20.
- Sigman-Grant M, Hayes J, VanBrackle A, Fiese B (2015) Family Resiliency: A Neglected Perspective in Addressing Obesity in Young Children. Child Obes 11:664-73.
- Teevale T, Kaholokula JK (2018) Using appreciative inquiry methodology to develop a weight management program for obese children in New Zealand. Aust N Z J Public Health 42:7-11.
- Morton SMB, Ramke J, Kinloch J, Grant CC, Carr PA, et al. (2015) Growing Up in New Zealand cohort alignment with all New Zealand births. Aust N Z J Public Health 39:82-7.
- Morton SM, Atatoa Carr PE, Grant CC, Robinson EM, Bandara DK, et al. (2012) Cohort profile: Growing up in New Zealand. Int J Epidemiol 42:65-75.
- Masten AS (2001) Ordinary magic: Resilience processes in development. Am Psychol 56:227-38.
- https://cdn.auckland.ac.nz/assets/growingup/research-findings-impact/report04.pdf
- Morton SMB, Carr PEA, Grant CC, Berry SD, Marks EJ, et al. (2014) Growing Up in New Zealand: A longitudinal study of New Zealand children and their families. Vulnerability Report 1: Exploring the Definition of Vulnerability for Children in their First 1000 Days. Auckland: Growing Up in New Zealand.
- Morton SMB, Carr PEA, Grant CC, Berry SD, Mohal J, et al. (2015) Growing Up in New Zealand: A longitudinal study of New Zealand children and their families. Vulnerability Report 2: Transitions in exposure to vulnerability in the first 1000 days of life. Auckland: Growing Up in New Zealand.
- Fergus S, Zimmerman MA (2005) Adolescent resilience: A framework for understanding healthy development in the face of risk. Annu Rev Public Health 26:399-419.
- Farewell CV, Thayer ZM, Puma JE, Morton S (2018) Exploring the timing and duration of maternal stress exposure: Impacts on early childhood BMI. Early Hum Dev 117:15-9.
- Masten AS, Coatsworth JD (1998) The development of competence in favorable and unfavorable environments: Lessons from research on successful children. Am Psychol 53:205-20.
- Duncan GJ, Brooks-Gunn J, Klebanov PK (1994) Economic deprivation and early childhood development. Child Dev 65:296-318.
- https://www.who.int/childgrowth/standards/Technical_report.pdf.
- Cole TJ, Lobstein T (2012) Extended international (IOTF) body mass index cutÃÆÃâÃââÃÆââ¬Å¡Ã¢ââ¬Å¡Ã¬ÃÆââ¬Å¡ÃâÃÂoffs for thinness, overweight and obesity. Pediatr Obes 7:284-94.
- Campbell K, Hesketh K, Silverii A, Abbott G (2010) Maternal selfÃÆÃâÃââÃÆââ¬Å¡Ã¢ââ¬Å¡Ã¬ÃÆââ¬Å¡ÃâÃÂefficacy regarding children's eating and sedentary behaviours in the early years: Associations with children's food intake and sedentary behaviours. Int J Pediatr Obes 5:501-8.
- McPhie S, Skouteris H, McCabe M, Ricciardelli LA, Milgrom J, et al. (2011) Maternal correlates of preschool child eating behaviours and body mass index: A crossÃÆÃâÃââÃÆââ¬Å¡Ã¢ââ¬Å¡Ã¬ÃÆââ¬Å¡ÃâÃÂsectional study. Int J Pediatr Obes 6:476-80.
- Cooklin AR, Lucas N, Strazdins L, Westrupp E, Giallo R, et al. (2014) Heightened maternal separation anxiety in the postpartum: The role of socioeconomic disadvantage. J Fam Iss 35:1497-519.
- Black K, Lobo M (2008) A conceptual review of family resilience factors. J Fam Nurs 14:33-55.
- Appelhans BM, Fitzpatrick SL, Li H, Cail V, Waring ME, et al. (2014) The home environment and childhood obesity in low-income households: indirect effects via sleep duration and screen time. BMC Public Health 14:1160.
- Boles RE, Halbower AC, Daniels S, Gunnarsdottir T, Whitesell N, et al. (2017) Family chaos and child functioning in relation to sleep problems among children at risk for obesity. Behav Sleep Med 15:114-28.
- Carter PJ, Taylor BJ, Williams SM, Taylor RW (2011) Longitudinal analysis of sleep in relation to BMI and body fat in children: The FLAME study. BMJ 342:d2712.
- DeMattia L, Lemont L, Meurer L (2007) Do interventions to limit sedentary behaviours change behaviour and reduce childhood obesity? A critical review of the literature. Obes Rev 8:69-81.
- Fulkerson JA, Larson N, Horning M, Neumark-Sztainer D (2014) A review of associations between family or shared meal frequency and dietary and weight status outcomes across the lifespan. J Nutr Educ Behav 46:2-19.
- Berge JM, Wall M, Hsueh TF, Fulkerson JA, Larson N, et al. (2015) The protective role of family meals for youth obesity: 10-year longitudinal associations. J Pediatr 166:296-301.
- Berge JM, MacLehose RF, Loth KA, Eisenberg ME, Fulkerson JA, et al. (2012) Family meals. Associations with weight and eating behaviors among mothers and fathers. Appetite 58:1128-35.
- Harbec MJ, Pagani LS (2018) Associations Between Early Family Meal Environment Quality and Later Well-Being in School-Age Children. J Dev Behav Pediatr 39:136-43.
- Anderson SE, Whitaker RC (2010) Household routines and obesity in US preschool-aged children. Pediatrics 125:420-8.
- Taylor RW, Gray AR, Heath AM, Galland BC, Lawrence J, et al. (2018) Sleep, nutrition, and physical activity interventions to prevent obesity in infancy: Follow-up of the Prevention of Overweight in Infancy (POI) randomized controlled trial at ages 3.5 and 5 y. Am J Clin Nutr 108:228-36.
- Bursac Z, Gauss CH, Williams DK, Hosmer DW (2008) Purposeful selection of variables in logistic regression. Source Code Biol Med 3:17.
- Taveras EM, Gillman MW, Pena MM, Redline S, Rifas-Shiman SL (2014) Chronic sleep curtailment and adiposity. Pediatrics 133:1013-22.
- Chen X, Beydoun MA, Wang Y (2008) Is sleep duration associated with childhood obesity? A systematic review and metaÃÆÃâÃââÃÆââ¬Å¡Ã¢ââ¬Å¡Ã¬ÃÆââ¬Å¡ÃâÃÂanalysis. Obesity 16:265-74.
- Buxton OM, Chang AM, Spilsbury JC, Bos T, Emsellem H, et al. (2015) Sleep in the modern family: Protective family routines for child and adolescent sleep. Sleep Health 38:A384-A385.
- Whitesell CJ, Crosby B, Anders TF, Teti DM (2018) Household chaos and family sleep during infants’ first year. J Fam Psychol 32:622-31.
- Miller AL, Kaciroti N, Lebourgeois MK, Chen YP, Sturza J, et al. (2014) Sleep timing moderates the concurrent sleep duration-body mass index association in low-income preschool-age children. Acad Pediatr 14:207-13.
- Haines J, McDonald J, O'Brien A, Sherry B, Bottino CJ, et al. (2013) Healthy habits, happy homes: Randomized trial to improve household routines for obesity prevention among preschool-aged children. JAMA Pediatr 167:1072-9.
- Pridham KF, Chang AS (1989) What being the parent of a new baby is like: Revision of an instrument. Res Nurs Health 12:323-9.